March 1, 2022
Written by: Marissa Maroni
According to the CDC, approximately three million Americans have an inflammatory bowel disease1. This estimate includes individuals with Crohn’s disease and ulcerative colitis who commonly experience abdominal pain, fatigue, and diarrhea, among other symptoms. These diseases are caused by a defective immune system that mounts an inappropriate immune response against the gut. Although some treatments for inflammatory bowel disease are available, there are still many things that are unknown about this disease.
Neuroimmune interactions (communication between the nervous and immune system) have been of particular interest as neuroimaging studies have shown that certain brain regions are activated during gut inflammation2. Despite these findings, a direct connection between the brain and gut inflammation had not been demonstrated. Researchers from the Israel Institute of Technology and others aimed to study the interaction between the brain and colon during an immune response3. Investigating neuroimmune interactions and identifying brain regions that mediate an immune response may lead to improved treatments for gut-related disorders. You can learn more generally about the gut-brain access in this PNK article!
Experimental setup: activity-dependent cell labeling
The scientists first wanted to see what region of the brain is activated during an immune response in the gut. To do this, they used genetically-altered mice called TRAP mice (transgenic targeted-recombination-in-active-populations) where neurons are labeled with a fluorescent marker when activated. TRAP mice are an incredibly useful genetic technique as previously scientists could only extrapolate a potentially relevant neuronal cell type during a given experiment. TRAP mice can capture the exact neuronal population that is activated during a particular stimulus.
The researchers used the TRAP mice and induced inflammation in the mouse’s colon using a chemical called dextran sulfate sodium. This chemical has previously been found to cause an inflammatory response that is similar to ulcerative colitis4. You may be wondering “If the TRAP mice label active neurons, how do they label neurons specifically activated during the induced colon inflammation?” The TRAP mice were designed so that active neurons fluoresce only when the mouse has a certain chemical administered via injections giving them the ability to control when active neurons are being labeled. Scientists injected this chemical before they induced gut inflammation so that the neurons that are activated by the gut inflammation are the only ones that fluoresce.
What brain region codes for gut inflammation?
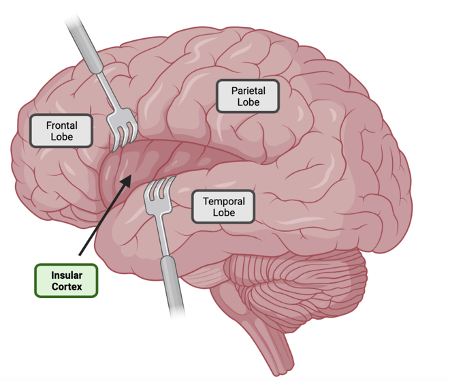
Utilizing this mouse model, the researchers found that a group of neurons in the insular cortex activated during colon inflammation. The insular cortex is deep inside your brain and is hidden underneath another brain region on the side of your head (Figure 1). This brain region is responsible for interoception, or perception of the internal body, and functions as a hub that integrates various inputs such as sensation, motivation, and cognition5. This result indicates that neuronal populations in the insular cortex detect inflammation in the colon. This result supports prior neuroimaging studies that identified increased insular cortex activity when individuals are experiencing inflammation2.
Can activating this brain region cause an immune response?
Researchers then wanted to demonstrate that the group of activated neurons in the insular cortex could produce inflammation in the colon. To achieve this, the scientists used chemogenetics to activate the specific neurons they observed responding to colon inflammation in their TRAP mice. They found that after activating these neurons, the colon had an increase in immune response cells, just like during the initial inflammation induced by the chemical. This builds upon the prior result as it demonstrates that activation of neuronal populations in the insular cortex can induce a colon immune response.
Is the insular cortex connected to the colon?
Up to this point, the researchers found that neuronal populations in the insular cortex are activated in response to colon inflammation and that reactivating this set of neurons can initiate a similar inflammatory state in the colon. Next, they wanted to see whether the insular cortex and the colon are connected directly or indirectly. Retrograde tracing, a technique that allows neuroscientists to see what neurons are connected to a brain region was used to check for a physical link between the gut and the brain. The researchers injected this tool into the colon to label cells that connect with this cell type in their TRAP mice. The researchers found that some of the neurons activated during inflammation were directly connected to cells labeled in the colon.
Can inhibiting this brain region lessen an immune response?
The goal in studying neuroimmune interactions is to produce new therapies for disorders such as inflammatory bowel disease. With this goal in mind, the scientists asked if they could lessen the immune response by reducing activity in the activated neuronal population in the insular cortex. This time, chemogenetics was used to inhibit instead of activate these neurons. By inhibiting this set of neurons in mice with induced inflammation, they found that the immune response in the colon was reduced! These findings illustrate where immune responses can be stored in the brain. Further, inhibition of insular cortex activity could be a new avenue for reducing colon inflammation! If you’re interested in learning more about gut to brain interactions check out this article on how stress can impact the gut!
References:
1. Centers for Disease Control and Prevention. (2021). Inflammatory Bowel Disease (IBD) in the United States. National Center for Chronic Disease Prevention and Health Promotion and Center for Disease Control and Prevention.
2. Sergeeva, M., Rech, J., Schett, G., & Hess, A. (2015). Response to peripheral immune stimulation within the brain: magnetic resonance imaging perspective of treatment success. Arthritis research & therapy, 17(1), 1-8.
3. Koren, T., Amer, M., Krot, M., Boshnak, N., Ben-Shaanan, T. L., Azulay-Debby, H., … & Rolls, A. (2021). Insular cortex neurons encode and retrieve specific immune responses. Cell, 184(24), 5902-5915.
4. Chassaing, B., Aitken, J. D., Malleshappa, M., & Vijay‐Kumar, M. (2014). Dextran sulfate sodium (DSS)‐induced colitis in mice. Current protocols in immunology, 104(1), 15-25.
5. Gogolla, N. (2017). The insular cortex. Current Biology, 27(12), R580-R586.
Photo by www_slon_pics from Pixabay
Figure 1 was created using BioRender
Leave a comment