October 18th, 2022
Written by: Lindsay Ejoh
Scroll to the bottom for a TikTok version of this post!
When you think of a placebo, you might imagine a “magic” pill that seems to cure diseases, even though it contains no active substance that affects health1. Placebos are not magic, but the belief or expectation that a treatment will work is enough to relieve symptoms along a variety of clinical conditions like depression, sleep disorders, menopause, allergies, and many others. One of the strongest placebo effects occurs during the treatment of pain, and is known as placebo analgesia, or expectation-driven pain relief2,3.
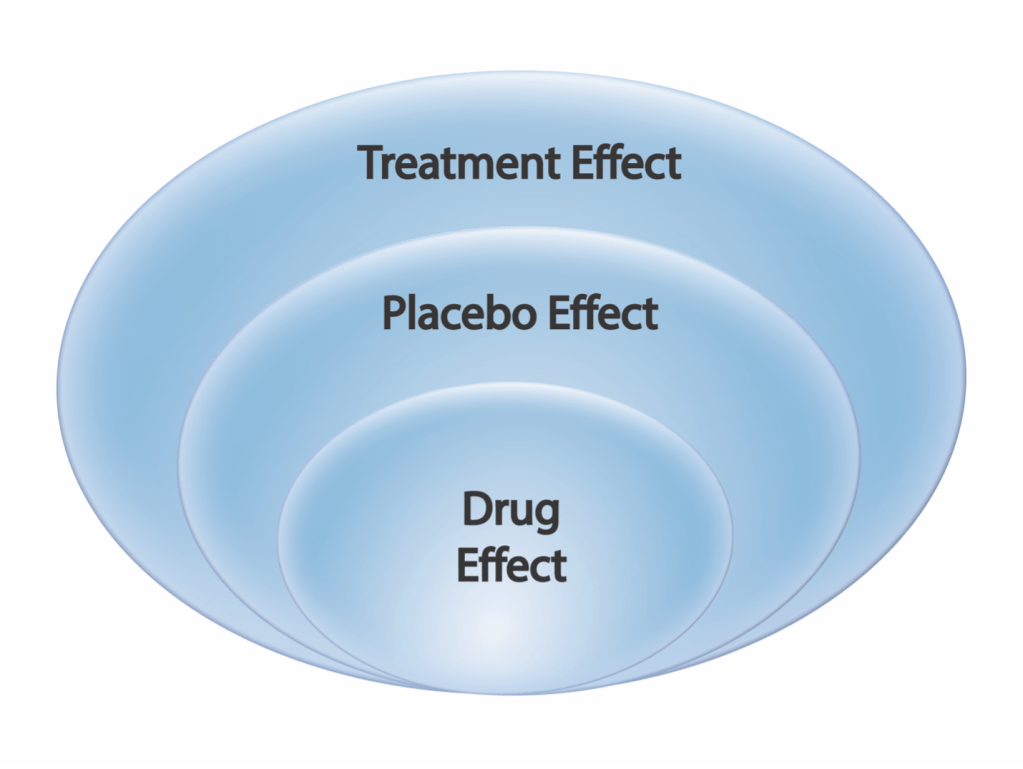
Placebo analgesia stems from the belief that a treatment will reduce or eliminate pain. This expectation can trigger the body to release neurotransmitters that block incoming pain signals from reaching the brain4. One important set of neurotransmitters released during placebo analgesia are endorphins, naturally-released opioid molecules that inhibit activity of pain-sensing neurons. (Learn more about the body’s natural opioid system and how they compare with opioid drugs in this previous NeuroKnow article). Placebo analgesia also involves release of other neurotransmitters like dopamine, which is commonly associated with motivation and reward, and cannabinoids, which are naturally-released molecules that have similar effects as cannabis drugs like THC and CBD5. The placebo effect is historically seen as the “bad guy” in clinical drug trials, since drug developers compare health outcomes of patients who get a real drug with those who get a fake, placebo treatment. In this case, the placebo effect is viewed as something the actual treatment is supposed to beat6. However, scientists are now beginning to see the placebo response as something that adds to a drug’s effectiveness, not something that combats it (Figure 1). Instead of pitting the drug effect against the placebo effect, the two are combined in a phenomenon known as the “treatment effect.” In this case, placebo interactions work together with a drug’s effect to improve patient outcomes.
Expectation and trust are very important factors in determining if a pain treatment will be successful11. Therefore, it is crucial for doctors to have realistic but positive attitudes when communicating with patients about their pain treatment options. When doctors are biased against patients, do not believe or validate their pain, and do not communicate enthusiastically about a particular pain treatment, a patient is at a greater risk of the treatment not being effective7.
Though surprisingly powerful, placebo analgesia is not always consistent. Certain people are more likely than others to be placebo responders3, and an individual placebo responder will not respond every time8. People who respond more to placebo tend to have differences in their brains’ opioid and dopamine systems, more agreeable or resilient personalities, and are more susceptible to hypnosis. Additionally, environmental cues are very important reinforcers of the placebo response. Placebo analgesia is more likely to occur when a patient is in conditions where they have had previous success in treating their pain9. For example, getting an injection-based treatment might help reduce pain more if that patient remembers that shots have helped them in the past more than pills.
Scientists are using what we know about the causes and mechanisms underlying placebo analgesia to create therapies that can ethically harness the placebo effect to help patients in pain. For example, researchers can use animal models to study how brains produce placebo analgesia and use what they learn to work towards creating therapies for human patients.
You may be wondering- if the pain you feel can be influenced by the environment and your expectations, does that mean the pain is all in your head? The answer is yes and no- pain is not imagined! The experience of pain is generated in the brain but is as real as ever. That’s why understanding how our brains alter our experience to relieve our pain could be such a powerful tool for future pain treatments.
References
- Saling, J. (2022, February 8). The placebo effect: What is it? WebMD. Retrieved October 11, 2022, from https://www.webmd.com/pain-management/what-is-the-placebo-effect
- Matthiesen, S. T., Lunde, S. J., Wohlert Kjær, S., Carlino, E., & Vase, L. (2019). Placebo analgesia effects across central nervous system diseases: what do we know and where do we need to go? Pain reports, 4(3), e717. https://doi.org/10.1097/PR9.0000000000000717
- Colloca, L., Klinger, R., Flor, H., & Bingel, U. (2013). Placebo analgesia: psychological and neurobiological mechanisms. Pain, 154(4), 511–514. https://doi.org/10.1016/j.pain.2013.02.002
- Levine, J. D., Gordon, N. C. & Fields, H. L. THE MECHANISM OF PLACEBO ANALGESIA. The Lancet 312, 654–657 (1978).
- Harvard Health Publishing. (2021, December 13). The power of the placebo effect. Harvard Health. Retrieved October 11, 2022, from https://www.health.harvard.edu/mental-health/the-power-of-the-placebo-effect
- Rafi, Z. (2018, October 28). We may not understand control groups. Less Likely. Retrieved October 11, 2022, from https://lesslikely.com/statistics/control-group-effects/#references
- Yetman, H. E., Cox, N., Adler, S. R., Hall, K. T., & Stone, V. E. (2021). What Do Placebo and Nocebo Effects Have to Do With Health Equity? The Hidden Toll of Nocebo Effects on Racial and Ethnic Minority Patients in Clinical Care. Frontiers in psychology, 12, 788230. https://doi.org/10.3389/fpsyg.2021.788230
- Kaptchuk, T. J., Kelley, J. M., Deykin, A., Wayne, P. M., Lasagna, L. C., Epstein, I. O., Kirsch, I., & Wechsler, M. E. (2008). Do “placebo responders” exist?. Contemporary clinical trials, 29(4), 587–595. https://doi.org/10.1016/j.cct.2008.02.002
- Price, D. D., Fillingim, R. B., & Robinson, M. E. (2006). Placebo analgesia: friend or foe? Current rheumatology reports, 8(6), 418–424. https://doi.org/10.1007/s11926-006-0035-1
- Cao, B., Liu, Y. S., Selvitella, A., Librenza-Garcia, D., Passos, I. C., Sawalha, J., Ballester, P., Chen, J., Dong, S., Wang, F., Kapczinski, F., Dursun, S. M., Li, X. M., Greiner, R., & Greenshaw, A. (2021). Differential power of placebo across major psychiatric disorders: a preliminary meta-analysis and machine learning study. Scientific reports, 11(1), 21301. https://doi.org/10.1038/s41598-021-99534-z
- IASP. (2022, August 3). Placebo and nocebo effects: The importance of treatment expectations and patient-physician interaction for treatment outcomes. International Association for the Study of Pain (IASP). Retrieved October 14, 2022, from https://www.iasp-pain.org/resources/fact-sheets/placebo-and-nocebo-effects-the-importance-of-treatment-expectations-and-patient-physician-interaction-for-treatment-outcomes/
Cover image made with Biorender.com by Lindsay Ejoh
