April 18, 2022
Written by: Sophie Liebergall
Cold may be the original medical therapy. According to the oldest known treatise on the treatment of traumatic injuries, a papyrus scroll dating back to 1600 BCE, ancient Egyptian physicians treated maladies ranging from skin infections to breast abscesses with “cold applications.”1 These “applications,” which were likely made of plants that caused a cooling sensation, are perhaps the first example of a systematic medical practice beyond spiritual rituals or prayers. The history of the therapeutic use of cold continued through the Ancient Greek physicians Hippocrates and Galen, who advocated for cold water as a means of stopping bleeding or bringing down fevers. Through the 18th and 19th centuries, cold baths were advertised as a cure-all that promoted general wellbeing and prevented contagion.2 But did you know that hypothermia is still used as a therapy to protect against brain injury in hospitals today?
When a person’s heart stops, the body is no longer able to pump blood, which carries oxygen to sustain the body’s organs. The brain, which is the most important organ (though we may be biased over here at PennNeuroKnow), is especially sensitive to this lack of oxygen. Even when doctors are able to restart the heart, the brain is often injured during the time in which the heart wasn’t pumping. One of the major ways that doctors try to protect the brain and help it heal after it is injured by lack of oxygen is to cool down the brain through a process called “therapeutic hypothermia.” To lower the temperature of the brain, doctors will cool down the whole body, usually by giving the patient an IV infusion of cold fluids and covering their skin with cooling devices.3
This whole-body cooling strategy has proved effective, but doctors and scientists have continued to research ways to improve the implementation of therapeutic hypothermia. Some doctors have developed a more targeted approach by only cooling the head with a helmet to try to avoid any damage that very low temperatures may cause to the body’s other organs.4 This strategy has been used for the spinal cord as well, where cold saline can be applied directly to the cord during surgery.5,6 Instead of cooling the patient from the outside, other scientists have tried to harness the brain’s innate ability to regulate the body’s temperature. Many drugs act on the brain’s temperature regulation mechanism, including natural hormones like neurotensin, anesthetics that are used to put patients to sleep during surgery, drugs that bind to opioid receptors, and even cannabinoids (molecules found in the cannabis plant, which have a role in the treatment of a number of neurologic disorders).7 Though the use of these cooling drugs is still limited to the research lab, there have been promising results in studies of pharmacologic hypothermia in large animals, especially when combined with external cooling methods.
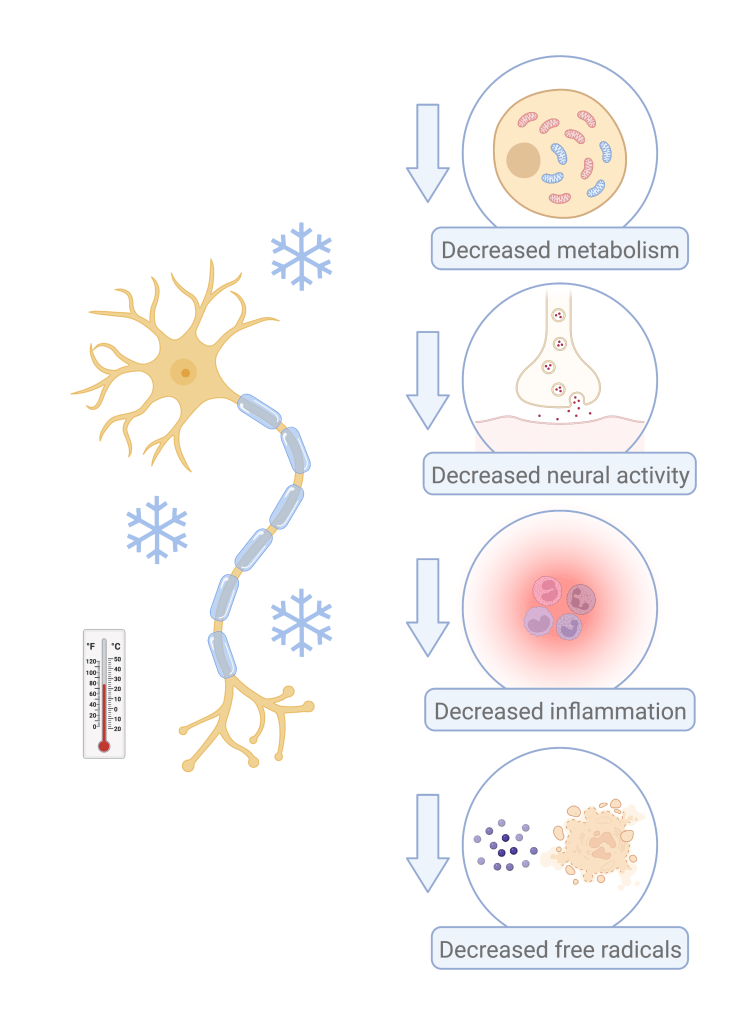
What exactly is happening in the brain when the temperature dips, and why does this help protect against brain injury? (Figure 1) Just as we like to stay at home snuggled under a blanket in the winter, cells tend to slow down in the cold as well. Neurons, which are the main cell type in the brain, slow their metabolism when they get cold.8 This means that they have a decreased demand for the oxygen and nutrients that are carried in the blood. Neurons also decrease their electrical activity in the cold.9 Electrical activity is the way in which neurons communicate with each other, allowing the brain to carry out its normal functions. But when neurons get too excited and start sending too many messages to each other, this can actually trigger reactions in the neuron that lead to its death. By slowing down electrical activity, cold can prevent this dangerous “excitotoxicity.”9
In the same way that you might put an ice pack on a swollen knee after an injury, cold may help dampen the inflammatory process in the brain as well. Cold has been shown to reduce the levels of some chemicals that recruit inflammatory cells to the site of an injury, while increasing the levels of other chemicals that calm down the inflammatory cells.10
Lastly, cold can decrease the generation of “free radicals” in the brain. Free radicals are highly reactive molecules that are generated normally during cell metabolism. However, when levels get too high, these molecules can wreak havoc in cells and cause damage to their inner structures. Inflammatory cells can make especially high levels of free radicals, which can injure neurons as well. Because cold both slows the normal generation of free radicals during metabolism and decreases the inflammatory response, cold may play a role in decreasing levels of free radicals following brain injury.11
Though we still have a long way to go in protecting patients from and helping them heal after brain injury, hypothermia is a relatively straightforward and effective therapy that was as intuitive to the ancients as it is to critical care physicians today. Future research will continue to explore different modalities of and protocols for therapeutic hypothermia, as well as test the efficacy of hypothermia in combination with other cutting-edge neuroprotective therapies, such as stem cell transplantation and targeted drug treatments.10
References:
- In Breasted, J. H., New-York Historical Society., & Stanton A. Friedberg, M.D. Rare Book Collection of Rush University Medical Center at the University of Chicago. (1930). The Edwin Smith surgical papyrus. Chicago, Ill: University of Chicago Press.
- Gianfaldoni, S., Tchernev, G., Wollina, U., Roccia, M. G., Fioranelli, M., Gianfaldoni, R., & Lotti, T. (2017). History of the Baths and Thermal Medicine. Open Access Macedonian Journal of Medical Sciences, 5(4), 566–568. https://doi.org/10.3889/oamjms.2017.126
- Mild therapeutic hypothermia to improve the neurologic outcome after cardiac arrest. (2002). New England Journal of Medicine, 346(8), 549–556. https://doi.org/10.1056/nejmoa012689
- Ikeda, K., Ikeda, T., Taniuchi, H., & Suda, S. (2012). Comparison of whole-body cooling and selective head cooling on changes in urinary 8-hydroxy-2-deoxyguanosine levels in patients with global brain ischemia undergoing mild hypothermia therapy. Medical science monitor : international medical journal of experimental and clinical research, 18(7), CR409–CR414. https://doi.org/10.12659/msm.883208
- Hansebout RR, Hansebout CR. Local cooling for traumatic spinal cord injury: outcomes in 20 patients and review of the literature. J Neurosurg Spine. 2014 May;20(5):550-61. doi: 10.3171/2014.2.SPINE13318. Epub 2014 Mar 14. PMID: 24628130.
- Bazley, F. A., Pashai, N., Kerr, C. L., & All, A. H. (2014). The effects of local and general hypothermia on temperature profiles of the central nervous system following spinal cord injury in rats. Therapeutic hypothermia and temperature management, 4(3), 115–124. https://doi.org/10.1089/ther.2014.0002
- Zhang, M., Wang, H., Zhao, J., Chen, C., Leak, R. K., Xu, Y., Vosler, P., Chen, J., Gao, Y., & Zhang, F. (2013). Drug-induced hypothermia in stroke models: does it always protect?. CNS & neurological disorders drug targets, 12(3), 371–380. https://doi.org/10.2174/1871527311312030010
- Patricia M. Schulte, Jason E. Podrabsky, Jonathon H. Stillman, Lars Tomanek; The effects of temperature on aerobic metabolism: towards a mechanistic understanding of the responses of ectotherms to a changing environment. J Exp Biol 1 June 2015; 218 (12): 1856–1866. doi: https://doi.org/10.1242/jeb.118851
- O’Leary, T., & Marder, E. (2016). Temperature-Robust Neural Function from Activity-Dependent Ion Channel Regulation. Current Biology, 26(21), 2935–2941. https://doi.org/10.1016/j.cub.2016.08.061
- Sun, Y. J., Zhang, Z. Y., Fan, B., & Li, G. Y. (2019). Neuroprotection by therapeutic hypothermia. Frontiers in Neuroscience, 13(JUN), 1–11. https://doi.org/10.3389/fnins.2019.00586
- Closa, D., & Folch-Puy, E. (2004). Oxygen Free Radicals and the Systemic Inflammatory Response. IUBMB Life (International Union of Biochemistry and Molecular Biology: Life), 56(4), 185–191. https://doi.org/10.1080/15216540410001701642