October 26, 2021
Written by: Nitsan Goldstein
Acupuncture has been used in China and other Asian countries for thousands of years. Today, acupuncture is widely used around the world to treat pain, nausea, and even psychiatric illnesses like anxiety and depression1. Acupuncture can also be used to treat inflammation, yet the mechanisms underlying its anti-inflammatory properties are not clear. Recently, a team of scientists from Harvard Medical School, Fudan University in Shanghai, and Meridians Research Center in Beijing discovered a pathway that could explain how stimulating certain points in the body can cause a body-wide decrease in inflammation through acupuncture2.
The research team’s work investigated the biological basis for the benefits of electroacupuncture, a specific method of acupuncture that involves placing thin needles into certain muscles, then attaching electrodes that deliver a small amount of electricity into the body through the needles. Using mice, the scientists first identified a protein, PROKR2, that is found in a subset of neurons in the dorsal root ganglia, or DRG. The DRG are bundles of neuronal cell bodies that extend out to the skin, muscles, or bones in one direction, and to the spinal cord in the other (Figure 1). DRG neurons are therefore critical in sending peripheral sensory information like touch, pain, or limb position to the spinal cord. PROKR2 was particularly interesting to the scientists because they noticed that the neurons that contained this protein sent dense projections to areas where electroacupuncture is especially successful at decreasing inflammation. For example, ST36 is an acupuncture point in the leg while ST25 is one in the abdomen. Electroacupuncture at low intensities can reduce inflammation when the needle is inserted in ST36, but not when it is inserted in ST25. PROKR2 DRG neurons send dense projections to the deep tissue in ST36, but much more sparse projections to ST25 tissue. Because of the link between the amount of PROKR2 innervation and the ability of electroacupuncture to reduce inflammation, the team decided to investigate the role of these DRG neurons.
The first step was to cause systemic (body-wide) inflammation in mice and then measure the effects of electroacupuncture on inflammatory and anti-inflammatory markers in the blood. To induce systemic inflammation, they injected a bacterial toxin called lipopolysaccharide (LPS). LPS causes an inflammatory response that can be quantified by measuring inflammatory markers in the blood. When electroacupuncture was applied to the mice’s hindlimbs, the amount of inflammatory markers in the blood was markedly reduced. What might cause the decrease in inflammatory markers? One possibility is the release of anti-inflammatory agents from the adrenal gland. Indeed, electroacupuncture increased blood levels of noradrenaline, adrenaline, and dopamine, which are anti-inflammatory molecules that are released by the adrenal glands (Figure 1). To test whether PROKR2 DRG neurons are necessary for the anti-inflammatory effects of electroacupuncture, the scientists ablated, or killed, all DRG neurons that contained PROKR2. Amazingly, electroacupuncture was no longer able to decrease inflammatory markers, and the increase in the anti-inflammatory molecules that are released by the adrenal glands was also gone. These results suggested that DRG PROKR2 neurons are essential for the anti-inflammatory effects of electroacupuncture.
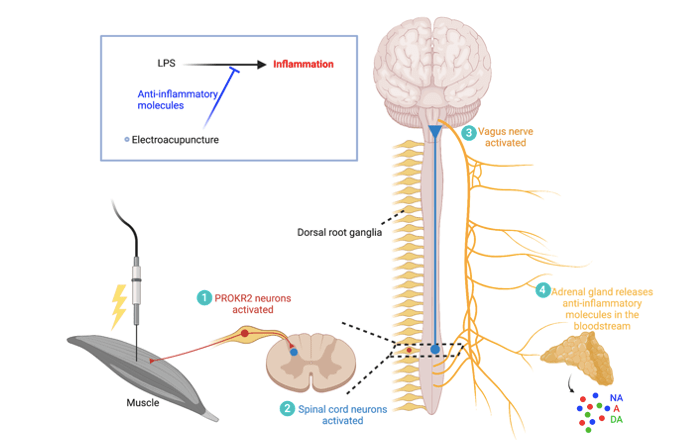
Now that the scientists knew that the DRG neurons are necessary for decreasing inflammation, they wondered whether activating them would also be anti-inflammatory. Through sophisticated genetic strategies, they used light to activate PROKR2 neurons in the ST36 region where electroacupuncture has strong anti-inflammatory effects. They found that optical activation of these neurons had effects that were very similar to electroacupuncture: increasing anti-inflammatory molecules like noradrenaline, adrenaline, and dopamine while decreasing inflammatory markers. They made another important discovery, however. The scientists found that the vagus nerve, a major highway of information between the brain and the rest of the body, was crucial for the effects of PROKR2 neuron stimulation on inflammation. When they severed the vagus nerve, PROKR2 activation was no longer able to affect systemic inflammation. This helped solidify the pathway through which electroacupuncture exerts its anti-inflammatory effects.
The authors of the study concluded that electroacupuncture activates PROKR2 DRG neurons that then project to the spinal cord. The spinal cord signal is transmitted to the brain, where cells bodies of the vagus nerve are activated. The vagus nerve then signals to the adrenal gland to release anti-inflammatory molecules into the bloodstream that act throughout the body to decrease inflammation (Figure 1). Remarkably, the scientists were able to predict where else in the body electroacupuncture would successfully decrease inflammation based on regions where PROKR2 neurons densely innervated the deep tissue. For example, they found that a different acupuncture point, LI10, in the forelimbs had abundant PROKR2 expression in the deep tissue while a set of muscles in the back of the legs did not. Electroacupuncture in LI10 was able to suppress inflammation while electroacupuncture in the back leg muscles was not. This groundbreaking work could go a long way in informing treatments for inflammatory diseases and potentially other disorders that are improved by acupuncture. It also reminds us that even with modern technology and advancements in medicine, we are still trying to figure out how treatments that were invented thousands of years ago are able to heal our bodies and minds.
References:
- Acupuncture: In Depth. (2016). National Center for Complementary and Integrative Health. https://www.nccih.nih.gov/health/acupuncture-in-depth
- Liu, S., Wang, Z., Su, Y., Qi, L., Yang, W., Fu, M., Jing, X., Wang, Y., & Ma, Q. A neuroanatomical basis for electroacupuncture to drive the vagal-adrenal axis. (2021) Nature. Epub ahead of print.
Cover image by 5petalpics from Pixabay https://pixabay.com/photos/acupuncture-holistic-healing-5126777/
Figure 1 created using BioRender
Leave a comment