October 13, 2020
Written by: Nitsan Goldstein
If you’ve ever had a surgical procedure, you’ve experienced the strange feeling of going under general anesthesia. General anesthetics cause loss of consciousness and make surgery tolerable. You might think, as most people do, that the procedure is not painful because you are unconscious. However, in rare cases, some patients are actually aware of what is happening during their surgery while under general anesthesia. Even in these cases, though, patients do not report being in pain1. These remarkable events suggest that anesthesia has the ability to potently suppress pain, and that this effect does not depend on the loss of consciousness that typically occurs. Scientists are trying to use this knowledge to find areas of the brain that can be targeted to treat pain more effectively. Recent work from researchers at Duke University has taken neuroscientists a step closer to this goal2.
Pain in the Brain
Pain is an extremely important adaptation that teaches humans and animals to avoid bodily harm. Chronic pain, however, is not advantageous and can cause other harmful conditions such as depression. Opioids are a commonly used class of drugs that are very effective in treating pain. Opioids are actually also produced by our bodies and act as one of the brain’s natural analgesic (pain-reducing) systems. The problem with opioids, however, is that the receptor for the compounds given as a pain reducer are present all over the brain, including in the brain’s reward system. Activation of this circuit by opioids is what makes this class of drugs highly addictive. Because of this, neuroscientists are trying to innovate new ways to treat pain that will be just as effective an analgesic as opioids while avoiding the off-target effects in the brain that can cause dependence and addiction.
To best understand how to treat pain, we must know how pain is signaled in the brain. The problem is that there is not one region in the brain that is solely activated during pain. Pain activates many regions across the whole brain, including areas in the back of the brain like the periaqueductal grey and the parabrachial nucleus, as well as regions in the front of the brain like the amygdala and anterior cingulate cortex3. How can we possibly target all of these regions to shut down pain? Instead of trying to quiet all these different pain promoting regions at once, can we instead activate a pain suppressing region in the brain that might have the same effect?
So where does anesthesia come in?
Inspired by this idea, a group at Duke University leveraged what we know about general anesthesia – that it is a powerful analgesic – to try to find a group of neurons in the brain that suppress pain2. To best find and manipulate these neurons, they used a mouse model. As you might expect, general anesthesia in mice substantially decreased neural activity in almost all areas of the brain. However, there was a small population of neurons in the central amygdala that were actually activated by general anesthesia. Could this be the region that suppresses pain under anesthesia?
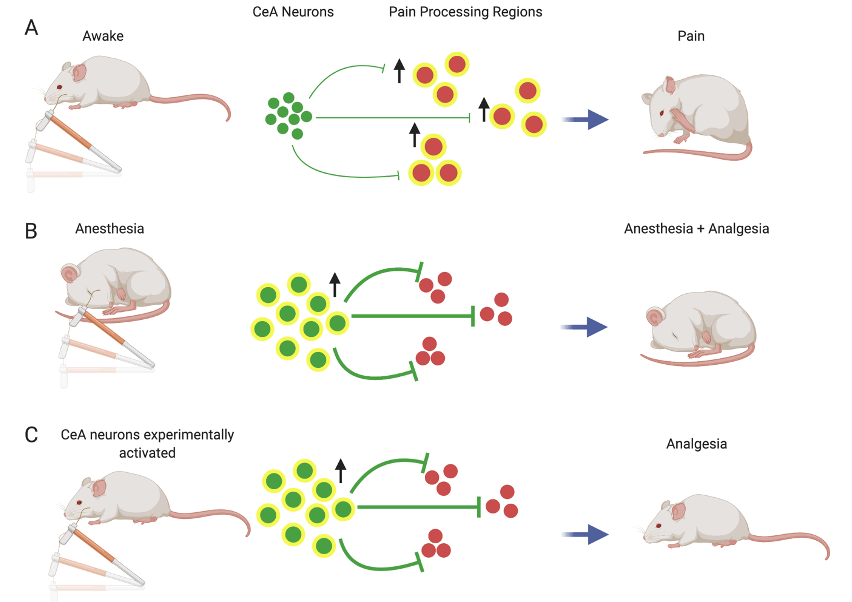
To find out, the group manipulated the activity of these central amygdala neurons that were activated by anesthesia. In some mice they enhanced the neural activity while in others they suppressed activity. They then administered unpleasant stimuli to the mice such as poking them with a metal filament or injecting a chemical into their paw that causes a burning sensation. Scientists can observe a mouse’s responses to these stimuli and infer the amount of pain they are in. When they activated the neurons in the central amygdala, the mice barely responded to the painful stimuli. When they inactivated the same neurons however, the mice had exaggerated pain responses to the stimuli. These incredible results showed that these neurons have the ability to suppress pain when activated, just as they are when animals are under anesthesia (see Figure 1).
The tests performed showed that the neurons can alter acute pain, where the stimulus is still present and directly causing pain. Many people, however, suffer from chronic or neuropathic pain. This kind of pain occurs long after an injury, for example, and reflects a resetting of the pain threshold such that previously non-painful stimuli become painful over time. The scientists wondered if these neurons could also suppress neuropathic pain when activated. To test this, they subjected the mice to a neuropathic pain model, where a nerve in the face is constricted. The effect is that stimuli that are normally not painful now cause the animal to withdraw and wipe their face – a sign that they are in pain. The scientists found that, when the central amygdala neurons were activated, the mice displayed this pain behavior less often than when they weren’t activated, suggesting that these neurons are also able to suppress chronic neuropathic pain.
Finally, the scientists wondered whether these neurons block pain by inhibiting other regions known to encode pain. They looked at the connections between the central amygdala neurons and the rest of the brain and found that they communicate with many of the areas known to be involved in pain processing. When the central amygdala neurons were activated, there was significantly less neural activity in these regions following a painful stimulus than when the neurons were not activated (see Figure 1). It is possible, then, that this relatively small population of neurons acts as a natural pain suppressor in the brain.
What’s next?
It is both interesting and potentially beneficial to understand the normal function of these central amygdala neurons. Anesthesia is not a natural phenomenon, so when do these pain-suppressing neurons normally activate? One possibility is that these neurons are activated during intense stress, which can cause analgesia. You’ve probably seen a tv show or movie featuring a severely injured person who feels no pain while they are “in shock” or full of adrenaline. The brain’s ability to dampen pain in situations where a person or animal needs to be very alert or be able to escape would be an obviously advantageous trait. It is possible that this neural circuit evolved to serve this function.
While these neurons did not evolve for the purposes of anesthesia, the fact that drugs such as isoflurane and ketamine can activate them is extremely important. It means that there are pharmacological (using drugs) ways to activate these neurons and suppress pain. Undoubtedly, future work will try to uncover exactly how these drugs can tap into this circuit, and how we may be able to create new drugs that will have the same effect on pain without the sedative side effects of anesthesia. The hope is that pain killers can be developed that specifically target this pain suppressing circuit, reducing the risk of addiction.
References
- Sebel, P. S. et al. Te incidence of awareness during anesthesia: a multicenter United States study. Anesth. Analg. 99, 833–839 (2004).
- Hua, T., Chen, B., Lu, D., Sakurai, K., Zhao, S., Han, B.X., Kim, J., Yin, L., Chen, Y., Lu, J., & Wang, F. General anesthetics activate a potent central pain-suppression circuit in the amygdala. Nat Neurosci. 23, 854-868 (2020).
- Peirs, C. & Seal, R.P. Neural circuits for pain: Recent advances and current views. Science 354, 578-584 (2016).
Cover Image by Tumisu from Pixabay
Figure 1 created using BioRender.com
Very interesting possibilities for managing chronic pain. Although it was not a major part of this article, I was interested to learn that mice wipe their faces when they are in pain. I wonder if, for cats, washing their faces is a self-comforting behavior. (I realize my comment is about as relevant to the main point as a fly on the head of a debater.)
LikeLike
That’s a great question! In this case, the mice are wiping their face in response to their face being poked- kind of like grabbing your toe when you stub it. There are other reasons for them to wipe, however, as you mentioned, like grooming (or to swat a fly away). As strange as it seems, mice actually make certain facial expressions when they are in pain that can be detected using high definition cameras (https://www.nature.com/articles/nmeth.1455). So there are ways to determine whether they are wiping to groom or because they are in pain. Over-grooming is actually a sign of stress in mice (and, it seems, also in cats!), so it certainly may provide some comfort in that context.
LikeLiked by 1 person