April 7, 2020
Written by: Greer Prettyman for IAES

Autoimmune encephalitis (AE) can be hard to diagnose because its symptoms can vary widely and may be similar to symptoms of other illnesses or disorders. When a patient is in the hospital with symptoms that may point to AE, they typically undergo a series of tests and evaluations to determine if a diagnosis of AE is likely. These test results help doctors decide whether or not to begin immunotherapy treatment, the normal standard of care for AE. Eventually patients get antibody testing to more precisely diagnose specific types of AE and refine treatment.
Typically, an MRI scan is included in the standard battery of tests when a patient with potential AE arrives at the hospital. MRI, magnetic resonance imaging, is a technique that uses a strong magnet to identify areas of the brain that may be overly active. Particular patterns of activity that can be seen with MRI, such as over activity in brain regions including the hippocampus, are often associated with AE1. However, many patients with AE have normal-looking MRIs, so MRI is not a perfectly accurate tool for diagnosis. A different type of diagnostic imaging called 18F-FDG PET might be able to detect certain types of encephalitis that would be missed with MRI1.
What is 18F-FDG PET?
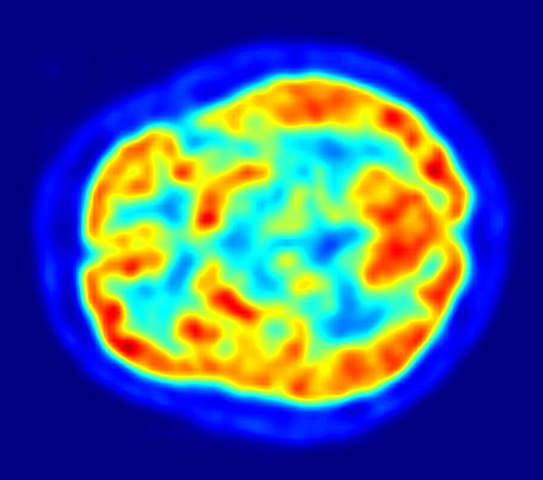
18F-FDG PET imaging, which stands for [18F]fluorodeoxyglucose positron emission tomography, uses a radioactively labeled glucose molecule to identify parts of the body or brain that have unusual amounts of activity. Glucose is the body’s main source of energy, so PET scans allow doctors to visualize areas that have high energy metabolism, or hypermetabolism. An area that is more active uses more glucose and shows up more strongly on a PET image. FDG PET is often used in cancer diagnosis because it can be used to locate parts of the body where cancer cells are growing and using a lot of extra energy2,3.
FDG PET imaging is also useful for identifying patterns of activity in the brain that are often associated with AE1,4. Many patients with a specific type of AE called limbic encephalitis who receive an FDG PET scan have hypermetabolism in a part of the brain called the medial temporal lobe5,6. This part of the brain is involved with emotion and memory, which are often altered as symptoms of AE. However, there is no one signature pattern that is consistently associated with limbic encephalitis, and other patients have shown patterns of unusually low metabolism in the medial temporal lobe or hypermetabolism in different brain regions, such as parietal and occipital lobes1,9.
Another subtype of AE called anti-NMDA receptor encephalitis may also be easier to diagnose with FDG PET than with MRI7. This type of encephalitis that affects NMDA glutamate receptors in the brain is often associated with hypermetabolism of glucose in the frontal and temporal lobes and hypometabolism in the occipital lobe7. A study at Johns Hopkins looked at PET and MRI scans of 5 patients with anti-NMDA receptor encephalitis and found that all 5 had abnormal PET scans but no abnormalities detected with MRI scans1.
Doctors have been able to diagnose these types of AE based on FDG PET results, even when that patient’s MRI scans appear normal4. One study of AE patients found that 85% had abnormal FDG PET scans, a greater percentage than for either MRI or EEG, suggesting that FDG PET may be a more sensitive measure8. For these reasons, researchers believe FDG PET may be an important tool for getting specific and precise diagnoses of AE6.
PET vs MRI
One drawback of using PET scans for early diagnosis is that they are typically not as quick and easy to obtain as an MRI. Many hospitals require time to schedule PET imaging so it cannot be completed when a patient is in the hospital with possible AE symptoms that need to be evaluated. MRI, on the other hand, can usually be performed on an emergency basis, so these results can be obtained more quickly and guide early treatment decisions10,11.
Another argument against implementing PET imaging as part of an initial battery of tests to diagnose AE is that a small amount of radiation is injected into the body in the form of the radioactive glucose tracer. However, many patients with AE symptoms already get PET scans of the body to check for tumors, so performing a PET scan of the brain at the same time would not require any extra radiation and would help doctors to get more information on what is going on in the brain6.
More research will be needed to determine exactly how accurate FDG PET can be at diagnosing different subtypes of AE, but since PET scans offer more precise diagnostic powers than MRIs, FDG PET shows promise as another tool to help with the diagnosis of AE.
References:
- Solnes, L. B., Jones, K. M., Rowe, S. P., Pattanayak, P., Nalluri, A., Venkatesan, A., … Javadi, M. S. (2017). Diagnostic Value of 18 F-FDG PET/CT Versus MRI in the Setting of Antibody-Specific Autoimmune Encephalitis. J Nucl Med, 58, 1307–1313.
- Gallamini, A., Zwarthoed, C., & Borra, A. (2014). Positron Emission Tomography (PET) in Oncology. Cancers, 6(4), 1821–1889.
- Shukla, A. K., & Kumar, U. (2006). Positron emission tomography: An overview. Journal of Medical Physics, 31(1)
- Deuschl, C., Rüber, T., Ernst, L., Fendler, W. P., Kirchner, J., Mönninghoff, C., … Umutlu, L. (2020). 18F-FDG-PET/MRI in the diagnostic work-up of limbic encephalitis. PloS One, 15(1).
- Baumgartner, A., Rauer, S., Mader, I., & Meyer, P. T. (2013). Cerebral FDG-PET and MRI findings in autoimmune limbic encephalitis: correlation with autoantibody types. Journal of Neurology, 260(11), 2744–2753.
- Morbelli, S., Djekidel, M., Hesse, S., Pagani, M., Barthel, H., Committee of the European Association of Nuclear Medicine, N., … Imaging, M. (2016). Role of 18F-FDG-PET imaging in the diagnosis of autoimmune encephalitis.
- Leypoldt, F., Buchert, R., Kleiter, I., Marienhagen, J., Gelderblom, M., Magnus, T., … Lewerenz, J. (2012). Fluorodeoxyglucose positron emission tomography in anti-N-methyl-D-aspartate receptor encephalitis: distinct pattern of disease. Journal of Neurology, Neurosurgery, and Psychiatry, 83(7), 681–686.
- Probasco, J. C., Solnes, L., Nalluri, A., Jesse Cohen, B., Krystyna Jones, B. M., Zan, E., … Venkatesan, A. (2017). Abnormal brain metabolism on FDG-PET/CT is a common early finding in autoimmune encephalitis. Neurol Neuroimmunol Neuroinflamm, 4, 352.
- Lee, S. K., & Lee, S.-T. (2016). The Laboratory Diagnosis of Autoimmune Encephalitis. Journal of Epilepsy Research, 6(2), 45–50.
- Graus, F., Titulaer, M. J., Balu, R., Benseler, S., Bien, C. G., Cellucci, T., … Dalmau, J. (2016). A clinical approach to diagnosis of autoimmune encephalitis. The Lancet.Neurology, 15(4), 391–404.
- Graus, F., & Dalmau, J. (2016). Role of 18F-FDG-PET imaging in the diagnosis of autoimmune encephalitis – Authors’ reply. The Lancet Neurology, 15(10), 1010.
Cover Image from Wikimedia, public domain via Jens Maus https://commons.wikimedia.org/wiki/File:PET-image.jpg
Thanks for your clear explanation of this difficult-to-diagnose disease, a disease that can cruelly steal a person’s memories.
LikeLike