May 29, 2018
Written by: Carolyn Keating
Do you ever think that you feel your phone vibrating in your pocket, then realize it’s not there? Well imagine if you thought that you felt your leg itch, but your leg wasn’t there! Feeling ghost sensations like these in a missing limb is a common occurrence for people who have undergone an amputation; in fact, up to 80% of amputees experience them1. But what exactly are these feelings, and how can amputees manage them?
After an amputation, people often feel as though their missing limb is still occasionally present. These phantom limb phenomena fall into two categories. The first is phantom sensations, in which amputees experience non-painful feelings such as warm and cold temperatures, itchiness, or tingling in their missing limb2. Although phantom limbs often have the same shape, length, and volume as the original body part, sometimes a phenomenon called telescoping can occur1. Here, the far end of the limb feels like it’s getting closer and closer to the body over time; for instance, someone with a leg amputation may first feel as though their foot is in its normal position, then shorten so the foot is where the knee would be, and may even reach the stump of the remaining part of the leg.
Although phantom sensations may be disconcerting, they rarely require medical attention. In contrast, the second category of phantom phenomena is much more debilitating, and is referred to as phantom pain. Here the sensations in the ghost limb have been described as shooting, stabbing, boring, squeezing, throbbing or burning, and usually seem to be coming from the part of this missing limb furthest from the body (like the hand or foot). The missing limb may also feel like it’s twisted into an uncomfortable position2.
What Causes These Sensations?
Despite reports of phantom limb pain existing for hundreds of years, scientists still aren’t completely sure why people feel sensations in limbs that are no longer present, but they do have some ideas. It seems like changes throughout the nervous system—the peripheral nerves of the body, the spinal cord, and the brain (Figure 1)—all contribute to experiencing phantom sensations and pain.
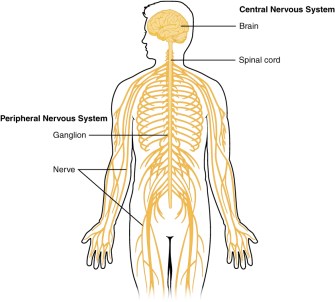
When a limb is amputated, the peripheral nerves in that region are cut. These nerves try to regrow in response to injury but are unable to do so correctly, creating a tangle of nerve endings. This ball of nervous tissue send signals to the brain both spontaneously and in response to pressure on the stump of the amputated limb, which the brain interprets as pain or other sensations. However, using anesthesia to block signals from the peripheral nerves does not always completely stop phantom limb pain, suggesting that other parts of the nervous system are also involved1,3.
In the spinal cord, neurons relay sensory information from the periphery to the brain. After a nerve injury—such as an amputation—spinal cord neurons that are responsible for transmitting pain information become more sensitive, meaning that they will fire more often and in response to input that would normally not be enough to evoke activity. Also contributing to this increased sensitivity is damage to inhibitory neurons that normally dampen down the firing of neurons that transmit pain information, and the abnormal firing of neurons that transmit other sensory information being interpreted by the brain as pain1,3.
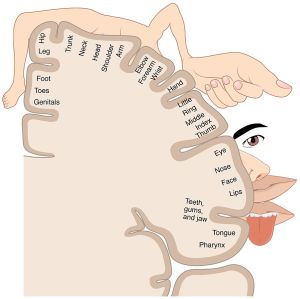
The brain itself also changes in response to an amputation. In the brain, each body part is represented in the primary somatosensory cortex (Figure 2), which is the brain region responsible for processing sensory information such as touch, pressure, pain, temperature, and position. The amount of cortex devoted to any one region is not proportional to how large that region is, but instead is based on how many neurons innervate the region. So body parts like the hands or face, which are very sensitive, have a larger representation than areas like the back. But what happens to these representations when a body part is amputated? Studies in adult monkeys showed that when the hand or forearm was amputated (as part of an injury treatment), the somatosensory cortex reorganized. The area of the cortex that once represented the hand was invaded by the neighboring areas of arm and face4. Similar changes have been found in humans, with greater reorganization associated with greater phantom pain5. But how exactly this reorganization leads to sensations of pain is still not known.
Is There Any Way to Treat Phantom Limb Pain?
Treating phantom limb pain can be difficult. Although there are no specific medications for phantom limb pain, drugs used to treat other conditions can be helpful for some people. For instance, antidepressants (specifically tricyclic antidepressants) may relieve pain by modifying the chemical messengers neurons use to communicate pain signals. Anticonvulsants, which are used to treat epilepsy, can also be used to quiet down overactive neurons to slow or prevent pain signals. Opioids can also sometimes control phantom pain. Finally, a certain class of anesthetics called NMDA receptor antagonists (which includes the drug ketamine) can have the effect of quieting down overactive neurons and blocking the transmission of pain signals2.
Non-medical treatments are also an option. In a procedure called transcutaneous electrical nerve stimulation, adhesive patches on the skin of the limb stump send a weak electrical current that interrupts or masks pain signals, preventing them from reaching the brain. Acupuncture can also be used to alleviate pain, as it’s believed that the fine needles inserted into the skin stimulate the release of the body’s natural pain-relieving endorphins2.
Another non-medical treatment is called mirror therapy. A patient views their existing limb in a mirror that is angled in such a way to make it appear as though the amputated limb exists, “tricking” the mind (Figure 3). The person can then move their intact limb while watching the mirror and imagining that they are actually watching the missing limb move. If the phantom limb is felt to be stuck in a twisted or frozen position, mirror therapy can be used to “move” it to a more natural alignment2,6. Extending this idea, current efforts are aimed at using virtual reality goggles to “trick” the brain into thinking a limb can move and manipulate objects.

Adjusting to life without a limb can be challenging, especially if the amputee is also experiencing phantom pain. While doctors still don’t know why some people develop pain and others don’t, research into how phantom pain is produced will hopefully lead to new therapies to help patients manage it.

Leave a comment