March 10th, 2026
Written by Omer Zeliger
In Stephen King’s 1981 horror novel, Cujo, the titular dog transforms from a friendly pet to a terrifying monster. He terrorizes his hometown and kills multiple people, but the real villain, the culprit for this inexplicable transformation, is the rabies that infected him1. Rabies has hung as a shadow over humanity for thousands of years2, often serving as inspiration for horror novels and zombie movies3. It’s easy to see why this virus is so feared. It drastically changes the behavior of the animals it infects, making them act aggressive and erratic. What’s more, it only needs a single bite or scratch to pass from an infected animal to a healthy one4-6. If left untreated, rabies is almost always fatal. Of the tens of thousands of people infected worldwide every year, only 31 have ever survived after the onset of symptoms7! But what exactly is rabies, and why does it have such a devastating effect on people who contract it?
Rabies transmission
Named after the Latin word rabere, meaning “to rage”, rabies is also known as “mad dog” syndrome, and its scientific name Lyssavirus comes from the Greek goddess of rage, Lyssa5,8. Most rabies victims will develop a set of symptoms known as “furious rabies”: becoming aggressive and foaming at the mouth4,6,9. These symptoms continue until the host is eventually killed by paralysis or a brain infection5,12. Scientists believe that rabies evolved these two characteristic symptoms in order to increase its ability to spread. Rabies is spread when infected saliva enters a wound4-6, which is much more likely when 1) the host is prone to biting, and 2) the host has plenty of infectious saliva in their mouth. Aggression makes the rabies victim more likely to bite, giving the virus a chance to infect a new host. Rabies infections also cause excessive drooling and a fear of drinking water6,9, increasing the amount of infectious saliva available and causing the distinct “foaming at the mouth” associated with rabid animals. Together, these symptoms make it more likely that rabies-infected saliva will get into an open wound, giving the virus a better chance of infecting a new host. This explains why rabies causes the symptoms it does, but not the how. How does rabies cause these drastic changes in behavior?
Infecting the brain
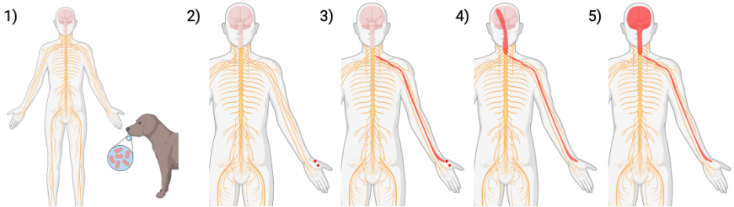
Before rabies can affect behavior, it has to travel from the bite wound to the brain. But the body protects the brain from diseases using the blood brain barrier, which stops harmful things like diseases from crossing over from the bloodstream to the brain. How does rabies bypass this protective barrier? Instead of trying to cross the well-protected path from blood vessels to the brain, rabies uses an alternative route: it travels along nerves. This “nerve pathway” is much less protected than the blood brain barrier – the nerves in your brain need to communicate with the nerves in your body, which means particles need to move freely between the two. The rabies virus takes advantage of this vulnerability by infecting nerves directly. First, rabies infects nerves in your body, such as the motor nerves that let you move your muscles10. These motor nerves are controlled by a series of nerves connected one to the next between the brain and body. Once the motor nerve is infected, the rabies virus works backwards, infecting the nerve that tells the motor nerve what to do, then infecting the nerve that tells that one what to do, and so on. By working backwards like this, rabies makes its way to the spinal cord, then works its way upwards until it reaches the brain (Figure 1).
This journey from the body to the brain can take anywhere from a week to a year, depending on where the bite happened and how much virus got into the wound6. During this period, rabies presents like any other infection – it might cause fever and pain or tingling at the bite wound. The more well-known rabies symptoms like rage and fear of drinking water come later, once the virus has reached the brain.
Rabies in the brain
Once rabies reaches the brain, it’s free to cause the behavioral changes it’s so well-known for, such as foaming at the mouth. To begin with, rabies causes its fear of water by “teaching” victims that drinking is painful4. It does this by causing the muscles in the throat to spasm painfully when the infected animal tries to swallow, eventually teaching the animal to avoid drinking water at all. This prevents the animal from washing out its saliva with water or swallowing extra saliva. On top of this, rabies infects the nerves controlling saliva production, causing them to go into overdrive and create even more infectious saliva11, all leading to the famous foaming of the mouth characteristic of rabies victims.
It’s less well understood how rabies causes aggression4. We can’t ask animals why they bite, but we can glean some insights from what humans experience in the late stages of rabies. Humans who contract rabies often exhibit an altered state of consciousness shortly before their death, and the confusion and fear from that experience may cause people to act aggressively12,13. One victim, for example, started experiencing delusions of being a famous soccer player. Within days his symptoms progressed; he became anxious and irritable, experienced delusions of persecution, and finally got into a fistfight with his brother12. Biologically, however, we still don’t know how rabies causes these changes.
Scientists have some ideas about the biological basis of rabies aggression, but we don’t know yet whether these ideas are correct. One possible explanation stems from recent research finding that a rabies infection forces the brain to produce a molecule similar to the neurotoxins found in snake venom14. Neurotoxins change how the brain functions and can cause altered states of consciousness, similar to how drugs like alcohol change our experience of the world. This neurotoxin-like molecule may be behind the delusions that rabies victims experience. Other research shows rabies damages various brain areas, including those involved in fear and anger15. Either or both of these processes, or even new processes we haven’t discovered yet, could contribute to the aggression so often seen in rabies victims.
Keeping yourself safe
One thing we know for sure about rabies is how deadly it is. How can you protect yourself from such a dangerous disease? As usual in health, the best cure is prevention. The vast majority of rabies cases in humans come from dog bites6, so vaccinating your pets is essential. Keep an eye out for wild animals acting strange. Most animals become aggressive when infected, but some can become paralyzed or even act overly friendly5. If you do happen to be bitten or scratched by an animal you suspect might have rabies, it’s important to get treatment as soon as possible. Rabies is nearly 100% fatal once symptoms start showing up, but if you act fast it can be treated with rabies antibodies and a post-exposure vaccine – survival rates of people who receive treatment within two days are almost 100%4,6,10.
Scientists have been hard at work researching potential treatments for rabies after symptoms have appeared, but so far have had little luck16. Ironically, the blood brain barrier that keeps us safe from so many other diseases may make it harder to treat rabies17. The blood brain barrier keeps medicines and even our own immune system from reaching the brain. Future treatments may investigate deliberately weakening the blood brain barrier in rabies patients. Unfortunately, like many proposed rabies treatments – including putting the patient in a medically-induced coma9 or lowering the patient’s body temperature7,16 – this puts an already-sick person in even greater danger. As our understanding of rabies improves, scientists may develop better treatments to help people survive infections. In the meantime, however, it’s better to be safe than sorry.
References
- King, S. (1981). Cujo. Viking Press.
- Tarantola A. (2017). Four Thousand Years of Concepts Relating to Rabies in Animals and Humans, Its Prevention and Its Cure. Tropical medicine and infectious disease, 2(2), 5. https://doi.org/10.3390/tropicalmed2020005
- Henkel, D., & Wijdicks, E. F. M. (2022). Cinema’s Terrifying Realities: Pandemics, Zombification, and SARS-COV-2. Clinical medicine & research, 20(3), 121–124. Advance online publication. https://doi.org/10.3121/cmr.2022.1742
- Mahadevan, A., Suja, M. S., Mani, R. S., & Shankar, S. K. (2016). Perspectives in Diagnosis and Treatment of Rabies Viral Encephalitis: Insights from Pathogenesis. Neurotherapeutics : the journal of the American Society for Experimental NeuroTherapeutics, 13(3), 477–492. https://doi.org/10.1007/s13311-016-0452-4
- Rupprecht, C. (2018, February). Rabies in dogs – dog owners. Merck Veterinary Manual. https://www.merckvetmanual.com/dog-owners/brain-spinal-cord-and-nerve-disorders-of-dogs/rabies-in-dogs
- World Health Organization. (2024, June 24). Rabies. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/rabies
- De Pijper, C. A., van Thiel, P. P. A. M., van de Beek, D., Brouwer, M. C., Aronica, E., Juffermans, N. P., Mathôt, R. A. A., GeurtsvanKessel, C. H., Schinkel, J., de Jong, M. D., Grobusch, M. P., & Goorhuis, A. (2025). Rabies in humans: A treatment approach. Travel medicine and infectious disease, 64, 102813. https://doi.org/10.1016/j.tmaid.2025.102813
- Etymologia: Rabies. (2012). Emerging Infectious Diseases, 18(7), 1169. https://doi.org/10.3201/eid1807.ET1807
- Hemachudha, T., Ugolini, G., Wacharapluesadee, S., Sungkarat, W., Shuangshoti, S., & Laothamatas, J. (2013). Human rabies: neuropathogenesis, diagnosis, and management. The Lancet. Neurology, 12(5), 498–513. https://doi.org/10.1016/S1474-4422(13)70038-3
- Ugolini G. (2011). Rabies virus as a transneuronal tracer of neuronal connections. Advances in virus research, 79, 165–202. https://doi.org/10.1016/B978-0-12-387040-7.00010-X
- Boonsriroj, H., Manalo, D. L., Kimitsuki, K., Shimatsu, T., Shiwa, N., Shinozaki, H., Takahashi, Y., Tanaka, N., Inoue, S., & Park, C. H. (2016). A pathological study of the salivary glands of rabid dogs in the Philippines. The Journal of veterinary medical science, 78(1), 35–42. https://doi.org/10.1292/jvms.15-0308
- Ferdaouss, Q., Boujraf, S., Ismail, C., Rim, E. A., Amine, B., Chadya, A., & Rachid, A. (2023). Rabies infection recognized as a psychosis: A misleading psychiatric presentation. Journal of neurosciences in rural practice, 14(3), 541–543. https://doi.org/10.25259/JNRP_20_2023
- Tongavelona, J. R., Rakotoarivelo, R. A., & Andriamandimby, F. S. (2018). Hydrophobia of human rabies. Clinical case reports, 6(12), 2519–2520. https://doi.org/10.1002/ccr3.1846
- Hueffer, K., Khatri, S., Rideout, S., Harris, M. B., Papke, R. L., Stokes, C., & Schulte, M. K. (2017). Rabies virus modifies host behaviour through a snake-toxin like region of its glycoprotein that inhibits neurotransmitter receptors in the CNS. Scientific reports, 7(1), 12818. https://doi.org/10.1038/s41598-017-12726-4
- Mohindra, R., Madhav, M., Suri, V., & Divyashree, K. (2022). Limbic system symptoms of rabies infection. BMJ case reports, 15(7), e249965. https://doi.org/10.1136/bcr-2022-249965
- Jackson A. C. (2013). Current and future approaches to the therapy of human rabies. Antiviral research, 99(1), 61–67. https://doi.org/10.1016/j.antiviral.2013.01.003
- Wang, L., Cao, Y., Tang, Q., & Liang, G. (2013). Role of the blood-brain barrier in rabies virus infection and protection. Protein & cell, 4(12), 901–903. https://doi.org/10.1007/s13238-013-3918-8
Header image by OpenClipart-Vectors on Pixabay
Figure created with Biorender.com

Leave a comment